Because of the potential complexity of rosacea and so little was known, for many years it was divided into subtypes according to signs and symptoms that often occur together. Although the cause of rosacea remains unknown, researchers now have a clearer understanding of how the disease develops and the processes involved in and under the skin. As a result, rosacea is now understood as a single disease with a wide variety of potential signs and symptoms (known as phenotypes.)1 A growing range of therapies is now available to address each of these signs and symptoms, and research and clinical experience have found that medications used in combination may have a synergistic outcome that is more effective than use of a single therapy alone. Accordingly, your doctor will tailor your treatment regimen to address your individual case.
As with any medical treatment, outcomes may vary from case to case. Compliance with therapy — using each medication exactly as your doctor prescribes — is an important key to success. Please consult a dermatologist or other physician to determine the appropriate regimen for you and how precisely to use it.
Therapeutic Options
Rosacea may now be diagnosed by the individual or combined presence of certain signs and symptoms. There are two diagnostic phenotypes — fixed centrofacial erythema (redness) and phymatous changes (skin thickening) — where the presence of either feature means the individual has rosacea. In the absence of a diagnostic phenotype, rosacea may also be diagnosed in the presence of two or more of the four major features: papules and pustules (bumps and pimples), telangiectasia (visible blood vessels), flushing and ocular rosacea (eye symptoms). Treatments targeted for individual phenotypes, alone or in combination, include a wide variety of topical and oral therapies as well as light devices and surgical interventions. An NRS Expert Committee recently assessed the various options according to effectiveness as well as the number of clinical studies.2 Please see the Management Options for Rosacea Patient Handout for details on the Committee’s opinion of the relative efficacy and strength of evidence for specific treatments mentioned below.
Diagnostic Phenotypes
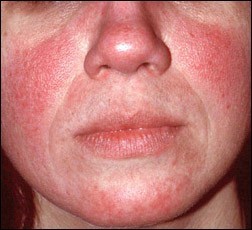 Persistent Redness
Persistent Redness
Persistent redness in the central part of the face (cheeks, nose, forehead and chin) that may come and go. In darker skin, erythema may look purple or brown.
Therapy: Clinical evidence for the topical FDA-approved therapies brimonidine and oxymetazoline was strong and effective, while oral antibiotic therapies were less often used for this feature. Light devices such as intense pulsed light (IPL), pulsed dye laser and potassium titanyl phosphate (KTP) laser may also be recommended.
Skin Thickening
Phymatous changes can include distended follicles (enlarged pores); skin thickening or fibrosis; glandular hyperplasia, or enlargement of the facial oil glands; and a bulbous appearance of the nose. Rhinophyma (thickening of the nose) is the most common form, but other thickening may occur elsewhere on the face. Phymas may be actively inflamed or fixed — that is, the result of earlier active inflammations that resulted in the thickened skin.
Therapy: For active cases with inflammation, topical retinoids are sometimes used in combination with oral therapies and/or treatments with surgical lasers. Other devices or surgical treatments, often in combination with other medical therapies, include the shaving off of excess tissue with a scalpel, electric current (electrosurgery) or radiofrequency waves that deliver intense heat to dermal tissue under the surface. Oral therapies, combined with the above treatments, may include isotretinoin and a range of antibiotics.
Treatment of the thickened skin of fixed phymas has been well studied and may often be effectively eradicated with a surgical laser or any of the other devices and/or surgical treatments mentioned above.
Major Phenotypes
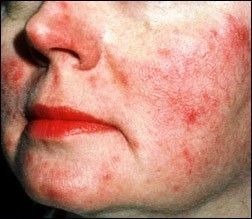 Bumps and Pimples
Bumps and Pimples
Dome-shaped red bumps (papules) with or without accompanying pimples (pustules), often in crops and primarily in the central facial area — the cheeks, nose, forehead and chin — are typical. Nodules or raised areas may also occur.
Therapy: FDA-approved topical therapies considered very effective include ivermectin, azelaic acid and metronidazole. Though with fewer clinical studies for rosacea, topical clindamycin, retinoids and sulfacetamide sodium/suler are also used. Oral therapies include a variety of antibiotics, including an FDA-approved low-dose version of doxycycline with less risk of microbial resistance (subantimicrobial doxycycline), as well retinoids.
Visible Blood Vessels
Tiny dilated or broken blood vessels (telangiectasia), sometimes called spider veins, often appear. These common signs are more visible in lighter skin, though they may still be present in darker skin.3
Therapy: Light devices such as IPL, pulsed dye laser and KTP laser have been well studied to rid the skin of visible blood vessels. Topical retinoids may occasionally be prescribed.
Flushing
Frequent and typically prolonged flushing (sometimes blushing) is common except in darker skin tones, in which case flushing may be subjectively experienced without obvious redness.
Therapy: The topical therapies brimonidine and oxymetazoline may be used, as well as antibiotics, alpha- and beta-blockers, IPL and, more rarely, KTP laser.
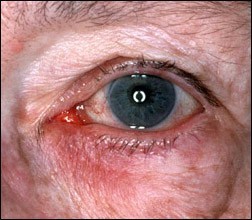 Eye Symptoms
Eye Symptoms
Ocular rosacea may appear as a spectrum of disease, from dry eye to blepharitis (inflammation of the eyelid) to meibomian gland dysfunction (dry eye), and may also include visible blood vessels on or around the eyelid margin; bloodshot eyes; spade-shaped hazy areas in the normally clear cornea; and redness and inflammation of the whites of the eyes. Common symptoms that may suggest ocular rosacea but are not specific to the disorder include burning, stinging, light sensitivity, and foreign object sensation.
Therapy: Topical therapies include antibiotics and the immunosuppressive therapies cyclosporin and tacrolimus. Oral antibiotics and IPL may also be used. Non-prescription treatment for mild to moderate ocular rosacea may include artificial tears and the daily cleansing of the eyelashes with baby shampoo on a wet washcloth.
Lifestyle Management
Because rosacea is characterized by flare-ups and remissions, its standard management options also include lifestyle changes and adjunctive care in addition to drug therapies and light devices. Some rosacea flareups may often appear to be initiated by environmental and lifestyle factors – often related to flushing as well as the development of bumps and pimples. Avoidance of the factors that affect you may help maintain remission.
Your doctor may advise you to keep a daily diary of lifestyle and environmental factors that appear to affect your rosacea to help identify and avoid your personal triggers. The most common factors are covered in Rosacea Triggers, and the NRS offers a Rosacea Diary to help you identify and avoid those factors that affect your individual case.
Skin Care
Gentle skin care and sun protection are important components of rosacea management. Patients with rosacea often have skin that is sensitive and easily irritated, causing redness, burning, and stinging, and sun exposure is one of the most common triggers for flare-ups. The goal of daily skin care is to maintain the integrity of the skin barrier while avoiding agents that aggravate inflammation or flushing. Visit the Skin Care & Cosmetics section for tips and recommendations.
References:
1. Gallo RL, Granstein RD, Kang S, et al. Standard classification and pathophysiology of rosacea: the 2017 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol 2018 Jan;78(1):148-155. doi: 10.1016/j.jaad.2017.08.037. Epub 2017 Oct 28.
2. Thiboutot D, Anderson R, Cook-Bolden F, et al. Standard management options for rosacea: The 2019 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol 2020; ;82(6):1501–1510. doi:10.1016/j.jaad.2020.01.077
3. Onalaja AA, Lester JC, Taylor SC. Establishing the diagnosis of rosacea in skin of color patients. Cutis 2019 July;104(01):38-41
Acknowledgment: This section was reviewed and edited by Dr. Zoe Draelos, consulting professor of dermatology, Duke University.