June 2004 • Volume 50 • Issue 6
Standard grading system for rosacea: Report of the National Rosacea Society Expert Committee on the Classification and Staging of Rosacea
Jonathan Wilkin, MD Chairmana
Mark Dahl, MDb
Michael Detmar, MDc
Lynn Drake, MDc
Matthew H. Liang MD, MPHd
Richard Odom, MDe
Frank Powell, MDf
Sections
- Classification of rosacea
- Grading of rosacea
- Conclusion
- Acknowledgements
- References
- From the Division of Dermatologic and Dental Drug Products, Food and Drug Administration, Rockville, Marylanda; Department of Dermatology, Mayo Clinic Scottsdale, Arizonab; Department of Dermatology, Harvard Medical School, Boston, Massachusettsc; Department of Medicine, Harvard Medical School, Boston, Massachusettsd; Department of Dermatology, University of California San Franciscoe; and Regional Centre of Dermatology, Mater Misericordiae Hospital, Dublin.f
- The opinions set forth in this report are those of the committee members and do not represent the Food and Drug Administration in any way.
- Reprint requests: The National Rosacea Society, 4619 N. Ravenswood Ave., Ste. 103, Chicago, IL 60640
-
J Am Acad Dermatol 2004;50:907-12.
- 01909622
- doi:10.1016/jaad.2004.01.048
INTRODUCTION
A standard classification system for rosacea was published in the April 2002 issue of the Journal of the American Academy of Dermatology.1 Developed by the National Rosacea Society Expert Committee on the Classification and Staging of Rosacea and reviewed by rosacea experts worldwide, it describes primary and secondary features of rosacea and recognizes 4 patterns of signs and symptoms, designated as subtypes. To enhance the utility of the system for both clinicians and researchers, the committee has devised a standard method for assessing gradations of the severity of rosacea. In addition to the classification system, a standard grading system is often essential to perform research, analyze results, and compare data from different sources, and in turn provides a common reference for diagnosis, treatment, and assessment of results in clinical practice. 2 and 3 Standard parameters and terminology also facilitate clear communication among a broad range of basic, clinical, and other researchers; practicing dermatologists; primary care physicians; ophthalmologists and other specialists; health and insurance administrators; and patients and the general public. The standard grading system rates the primary and secondary features of rosacea established by the standard classification system, and provides a global assessment of subtypes by both the physician and the patient. Beyond clinical manifestations, additional factors are important in determining the severity of rosacea from the patient's viewpoint. These may include the psychological, social, or occupational effects of the disorder,4 and other potential factors such as responsiveness to treatment.
For optimal utility, the grading system is designed to be reproducible and easily performed based on observation in clinical practice, while forming a consistent framework for more comprehensive measurements that may be developed for specific research studies. Moreover, as with the standard classification system, this grading system is an investigative instrument that can be readily modified based on clinical experience or updated and expanded as new discoveries are made.
CLASSIFICATION OF ROSACEA
Rosacea is a chronic cutaneous disorder affecting primarily the convexities of the central face (cheek, nose, chin, and central forehead). It is a syndrome or typology encompassing various combinations of signs and symptoms. In most cases, some rather than all of these features appear in any given patient, and they are often characterized by remissions and exacerbations. 5 and 6 The committee based the standard classification system on current scientific knowledge and morphologic characteristics to avoid assumptions on pathogenesis and progression, which are at present incompletely understood. As knowledge increases, the definition of rosacea may ultimately be based on causality rather than on morphology alone.
The committee first identified primary and secondary features of rosacea, and then delineated subtypes based on the most common patterns or groupings of these features. The primary signs of rosacea include flushing (transient erythema), nontransient erythema, papules and pustules, and telangiectasia. The presence of one or more of these features with a central face distribution is indicative of rosacea. Secondary features, which often appear with one or more of the primary features but can occur independently, include burning or stinging, plaques, dry appearance, edema, ocular manifestations, peripheral locations, and phymatous changes.
GRADING OF ROSACEA
For clinicians assessing patients, primary signs and symptoms may be graded as absent, mild, moderate, or severe (0-3), and most secondary features may be graded simply as absent or present (Table I). Researchers are encouraged to provide more detailed assessments. In some situations, more detailed or finer distinctions, perhaps supplemented by advanced technology, might be possible. Certain clinicians also may wish to use some of these other more comprehensive analytic methods, especially when based on visual observation.
Table I. Rosacea clinical scorecard
Flushing (transient erythema) Clinically, physicians should determine the presence or absence of flushing through patient history, and may ask about frequency, duration, extent, and severity. Noting the presence or absence of accompanying sweating may also be helpful. Perimenopausal flushing should not be considered significant unless it is accompanied by other characteristics of rosacea. Researchers may grade flushing from 0 to 3 based on intensity and frequency. In addition, duration of flushing may be noted, because some episodes are very transient (eg, from embarrassment) and some are not (eg, from ingestion of alcohol). Specific time frames may also be identified.
Nontransient erythema
For clinicians, nontransient (persistent) erythema may be graded from 0 to 3. Although inflammation (papules, pustules, plaques) or dry appearance may obscure the level of erythema, underlying redness should be evaluated disregarding this effect. Inflammation or dry appearance may be noted, but perilesional erythema should not be included in this assessment. In clinical studies, researchers may use instruments or other measurements to score erythema beyond a score of 0 to 3. For example, erythema may be assessed objectively with an appropriate device.
Papules and pustules
A modified version of the descriptive grading system established for acne vulgaris is recommended and shown in Table II. 7 Few to several papules and pustules, with no plaques, are scored as "mild." Several to many papules and pustules, with no plaques, are considered "moderate." Numerous and/or extensive papules and pustules, with or without plaques, are considered "severe." Table II. Severity grading of rosacea papules and pustules

Researchers should record the number of papules and pustules, and note the presence or absence of plaques.1
Telangiectasia
Telangiectasia may be graded in the clinical setting from 0 to 3. If erythema is intense, it may be difficult to definitively score telangiectasia, because erythema may mask some telangiectases, which become more visible if redness fades. This phenomenon has been described as posterythema-revealed telangiectasia.5 On the other hand, the presence of one or two isolated telangiectases in the absence of any other primary signs of rosacea may be insufficient for a diagnosis. Researchers also should count telangiectases, if feasible, at least in specified areas. Nasal and malar telangiectases should be identified independently, and be qualitatively described as fine and threadlike to coarse.
Secondary features
Burning or stinging In the clinical setting, burning or stinging may be reported by the patient and, if present, may be weighed into the overall assessment of severity. Researchers should seek out this information, record the locations of both symptoms if present, and use a systematic method of assessing both symptoms.
Plaques
In clinical practice, plaques may be noted. Plaques may be defined as confluent areas of inflammation, often seen as larger red areas among papules and pustules without epidermal changes in the surrounding skin. In research studies, they may be further differentiated by severity, location, or other criteria.
Dry appearance
In clinical practice, rough, dry-appearing skin may be noted. In research, this may also be stratified based on such criteria as distribution and severity. If scaling is noted, it may represent coexisting seborrheic dermatitis or irritation.
Edema
In clinical practice, edema may be identified by location (eg, periorbital, glabellar, malar) through patient history and examination. If present, it may be noted as acute, chronic recurrent, or chronic persistent and, if chronic, as pitting or nonpitting. Researchers may assign a grade of 0 to 3 according to extent and degree of swelling.
Ocular manifestations
Clinicians may identify ocular manifestations by looking for tearing, redness of bulbar and/or palpebral conjunctivae, telangiectasia of conjunctiva and lid margin, lid or periocular erythema, or styes, and by inquiring about symptoms of foreign-body sensation, gritty feeling, burning, stinging, itching, dryness, light sensitivity, blurred vision, or decreased visual acuity.8 Cases that are moderate to severe, progressive, or not responding to treatment, or where vision is affected, may require an ophthalmologic consultative approach. Treatment of cutaneous rosacea alone may be inadequate to reduce the risk of vision loss. 9 Researchers may wish to stratify the ocular manifestations as mild (signs/symptoms affecting eye margin, meibomian gland), moderate (signs/symptoms affecting inner lid, fluid secretion, eye surface), or severe (corneal damage and potential vision loss).
Peripheral location
Clinicians and researchers may determine the presence of any extrafacial signs and symptoms, and note the anatomic sites. Common extrafacial locations may include the neck, chest, scalp, ears, and back. The diagnosis of rosacea in locations other than the face may be problematic in the absence of diagnostic clinical or histologic features.
Phymatous changes
In the clinical setting, severity may be rated from 0 to 3, with 1 being patulous follicles but no contour changes, 2 being a change in contour without a nodular component, and 3 indicating a change in contour with a nodular component. Researchers may also note any vascular findings or inflammatory changes.
Global assessment of subtypes
Because the potential manifestations of rosacea are so numerous and varied, the committee concluded that global assessment can be most easily and meaningfully performed by subtype. The standard classification system established the following subtypes of rosacea, which are described in depth in the standard classification system.1 The following descriptions include the minimum signs and symptoms required to diagnose each subtype, and patients may have characteristics of more than one rosacea subtype at the same time.
Subtype 1: erythematotelangiectatic rosacea
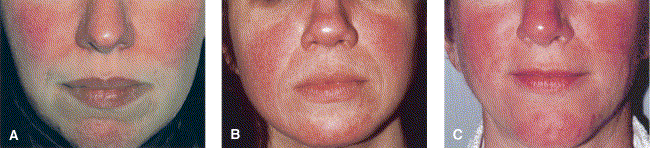
Subtype 1 (Fig 1) is characterized by flushing and persistent central facial erythema. Telangiectases are common but not essential for the diagnosis.
Fig 1. Subtype 1, erythematotelangiectatic rosacea, is characterized by flushing and persistent central facial erythema. Telangiectases are common but not essential for diagnosis. A, Mild; B, moderate; C, severe.
Subtype 2: papulopustular rosacea
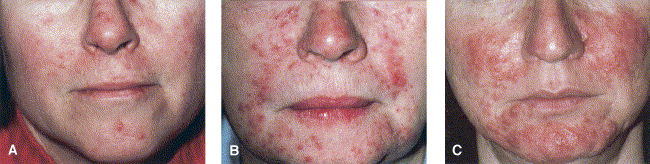
Subtype 2 (Fig 2) includes persistent central facial erythema with transient papules, pustules, or both in a central facial distribution. Burning and stinging may also be reported.
Fig 2. Subtype 2, papulopustular rosacea, includes persistent central facial erythema with transient papules, pustules, or both in central facial distribution. A, Mild; B, moderate; C, severe.
Subtype 3: phymatous rosacea
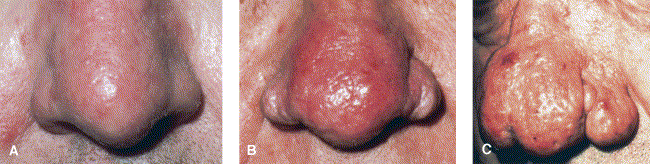
This subtype (Fig 3) may include thickening skin, irregular surface nodularities, and enlargement. Phymatous rosacea occurs most commonly as rhinophyma but may appear elsewhere, including the chin, forehead, cheeks, and ears. Patulous, expressive follicles may appear in the phymatous area, and telangiectases may be present.
Fig 3. Subtype 3, phymatous rosacea, may include thickening skin, irregular surface nodularities, and enlargement. Patulous, expressive follicles may appear in phymatous area, and telangiectases may be present. A, Mild; B, moderate; C, severe.
Subtype 4: ocular rosacea
Ocular rosacea (Fig 4) may include watery or bloodshot appearance (interpalpebral conjunctival hyperemia), foreign-body sensation, burning or stinging, dryness, itching, light sensitivity, blurred vision, telangiectasia of the conjunctiva and lid margin, or lid and periocular erythema. Blepharitis, conjunctivitis, and irregularity of the eyelid margins also may occur. Meibomian gland dysfunction presenting as chalazion, or chronic infection as manifested by hordeolum (stye), are common. Some patients may experience loss of vision as a result of corneal complications (punctate keratitis, corneal infiltrates, ulcers, or marginal keratitis). An ophthalmologic consultative approach to treatment may be required.
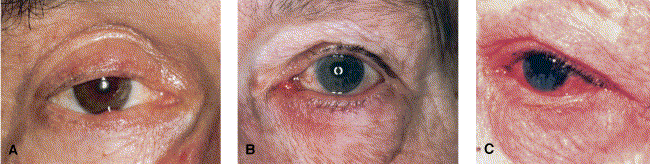
Fig 4. Subtype 4, ocular rosacea, may include watery or bloodshot appearance, telangiectasia of conjunctiva and lid margin, or lid and periocular erythema. Blepharitis, conjunctivitis, and irregularity of eyelid margins also may occur. A, Mild; B, moderate; C, severe.
For clinicians, global assessment for each subtype should be performed with a standard rating of 0 to 3, based on a composite of the severity of the signs and symptoms. The evaluation may also take into consideration the duration of signs and symptoms through patient history, and their extent at time of examination. For researchers, additional detail and assessment technology may be added beyond the basic rating system to provide further data and precision. The committee noted that the ultimate goal of diagnosis and treatment of rosacea is both to control the disorder and to minimize the discomfort of the patient. Patient participation in evaluation is, therefore, essential. The patient may provide a 0 to 3 global assessment of the severity of their condition in general terms that encompasses both the physical manifestations of rosacea and its impact on quality of life, which may include psychological, social, and occupational effects.
Patients might be informed of potential primary and secondary features of rosacea before their global assessments to aid them in evaluating their individual conditions more thoroughly. Of particular concern is ocular rosacea, which patients may not associate with cutaneous rosacea and that may require further evaluation.
CONCLUSION
In developing a standard grading system for rosacea, the committee attempted to design a basic examination process that is practical, useful, and similar to the usual examinations currently performed in clinical practice. To aid clinicians in evaluating their patients, the committee has developed a standard diagnostic flow chart (Table I). Superimposed on this basic standard system, researchers are encouraged to study and explore features beyond the minimum, using more sensitive and reproducible systems and applying new technology and methodologies that may further advance the scientific knowledge of rosacea. This investigational instrument is intended to help provide a foundation for better understanding of rosacea among practitioners and researchers by establishing a common language for communication and facilitating the development of a research-based approach to diagnosis and treatment. The scorecard (Table I) is included for those who wish to have a more detailed investigative record of the patient's disorder.
As with the standard classification system, this grading system is considered provisional and is subject to modification as the pathogenesis and subtypes of rosacea become clearer, and as its relevance and applicability are tested by investigators and clinicians. The National Rosacea Society Expert Committee welcomes comments on the usefulness and limitations of these criteria.
ACKNOWLEGEMENTS
The committee thanks the following individuals who reviewed and contributed to this document: Dr Joel Bamford, Department of Dermatology, St Mary's/Duluth Clinic, Duluth, Minnesota; Dr Mats Berg, Department of Dermatology, Uppsala University, Uppsala, Sweden; Dr Joseph Bikowski, Department of Dermatology, University of Pittsburgh, Pittsburgh, Pennsylvania; Dr Albert Kligman, Department of Dermatology, University of Pennsylvania, Philadelphia, Pennsylvania; Dr Ronald Marks, Department of Dermatology, University of Wales Medical Center, Cardiff, United Kingdom; Dr Gerd Plewig, Department of Dermatology, Ludwig-Maximilians University, Munich, Germany; Dr Bryan Sires, Department of Ophthalmology, University of Washington, Seattle, Washington; Dr Diane Thiboutot, Department of Dermatology, Pennsylvania State University, Hershey, Pennsylvania; Dr Guy Webster, Department of Dermatology, Thomas Jefferson University, Philadelphia, Pennsylvania; and Dr Mina Yaar, Department of Dermatology, Boston University, Boston, Massachusetts. The final document does not necessarily reflect the views of any single individual, and not all comments were incorporated.
The National Rosacea Society is a 501(c)(3) nonprofit organization whose mission is to support rosacea research, including the awarding of research grants, and to provide educational information on rosacea to physicians, patients, and the public. Reports or inquiries should be directed to the National Rosacea Society, 4619 N. Ravenswood Ave., Suite 103, Chicago, IL 60640; telephone 1-888-662-5874; E-mail: info@rosacea.org.
REFERENCES
1. Wilkin J, Dahl M, Detmar M, Drake L, Feinstein A, Odom R, et al. Standard classification of rosacea: report of the National Rosacea Society expert committee on the classification and staging of rosacea. J Am Acad Dermatol 2002;46:584-7.
2. C.E. Gessert and J.T.M. Bamford, Measuring the severity of rosacea: a review. Int J Dermatol 42 (2003), p. 444.
3. Henderson CA, Charles-Holmes S, McSween R, Ilchyshyn A. A system for grading rosacea severity. Br J Dermatol 1995;133(Suppl):34
4. Drake L. Rosacea takes emotional toll. Rosacea Rev 1998;summer:2.
5. J.K. Wilkin, Rosacea: pathophysiology and treatment. Arch Dermatol 130 (1994), pp. 359-362.
6. G. Plewig and A.M. Kligman, Editors, Acne and rosacea (3rd ed.), Springer, Berlin (2000).
7. Pochi PE, Shalita AR, Strauss JS, Webster SB. Report of the consensus conference on acne classification. J Am Acad Dermatol 1991;24:495-9.
8. Macsai MS, Mannis MJ, Huntley AC. Acne rosacea. In: Eye and skin disease. Philadelphia: Lippincott-Raven; 1996. p. 335-41.
9. E.K. Akpek, A. Merchant, V. Pinar and C.S. Foster, Ocular rosacea: patient characteristics and follow-up. Ophthalmology 104 (1997), pp. 1863-1867.
Reprint requests: National Rosacea Society, 4619 N. Ravenswood Ave., Ste. 103, Chicago, IL 60640, USA.
*1 Supported by the National Rosacea Society. Conflicts of interest: None identified. The opinions set forth in this report are those of the committee members and do not represent the Food and Drug Administration in any way.
*2 The National Rosacea Society is a 501(c)(3) nonprofit organization whose mission is to support rosacea research, including the awarding of research grants, and to provide educational information on rosacea to physicians, patients, and the public.